 Health Conditions and Omega 3
Health Conditions and Omega 3
This webpage covers 45+ health conditions and omega 3. Data from studies, benefits and research is included.
There have been many more studies conducted on the benefits of omega 3s in various journals and papers. Click here to view more studies.
Health Conditions and Omega 3 will be updated as more information becomes available.
For study information involving 42 children with learning disorders (including autism), click here for the Clinical Study Presentation.
Health Conditions and Omega 3 List
Acne, Aging, Aids, Allergies, Alzheimer’s, Angina, Arteriosclerosis (Artery Hardening), Arthritis, Asthma, Atopic Dermatitis, Attention Deficit Disorder, Autism, Autoimmune Diseases
Cancer, Cardiovascular Disorders, Crohn’s Disease, Cystic Fibrosis
Depression, Diabetes, Dyslexia, Dysmenorrhea (Menstrual Cramping)
Heart Disease, High Blood Pressure, Hyperactivity (ADHD)
Learning Disorder, Ligament Injuries, Lupus
Macular Degeneration, Menopause, Mental Illness, Multiple Sclerosis
Pregnancy, Prostate Cancer, Psoriasis
Raynaud’s Disease, Rheumatoid Arthritis
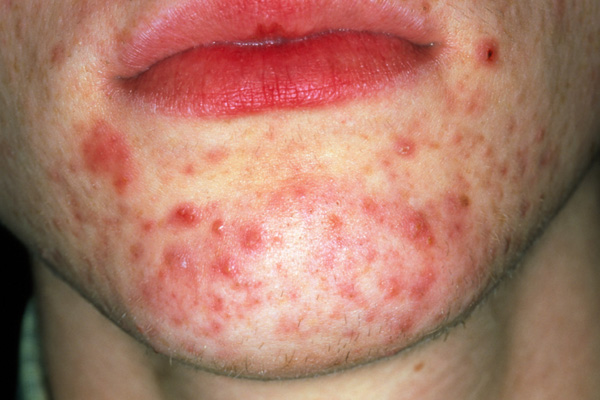 Acne
Acne
Many people who begin to use higher grade edible omega oils are amazed at the difference in their skin. They find that their skin feels creamy, supple, soft, and lovely to the touch. Hard skin, greasy pores, zits, bumps and acne disappear. These are the most obvious changes that many people notice on using good oils along with balanced nutrition. They also get an enhanced feeling of well-being.
Go to top of page.
Aging
No one wants to look older than his or her age. But if your skin is full of premature sags and wrinkles, you cannot avoid it. You may not think of your skin as an organ, but it is actually the largest organ in your body. Your skin has an extremely critical role to play as it provides a barrier against a very hostile environment that includes bacteria, fungi, and perpetual oxidation caused by the sun. Furthermore, aging is an important factor in the appearance of autoimmune disease. The immune system may be suppressed or weakened as a result of factors such as over-indulgence of alcohol, caffeine, tobacco, drugs, sugars and of course poor diet and lack of sleep.
Your skin’s appearance is a window to the internal state of your body. As you know, when you look good, it is usually when you are feeling strong and healthy. When your skin has a rosy glow, this means that good blood circulation is occurring within the skin and probably through the rest of your body. On the one hand, you often know you are getting sick when you see pallor to your skin, indicative of poor blood flow. You can bet that the rest of your body is not too far behind.
One unmistakable sign of aging is the formation of wrinkles. Scientifically speaking, wrinkles are caused by the cross-linking of collagen fibers in the skin, and the cross-linking can be accelerated by inflammation caused by the constant exposure to the sun.
The most effective way to reduce wrinkle formation (other that staying completely out of the sun) is to reduce Arachidonic acid (omega 6) levels in the skin, thus decreasing the potential for the production of pro-inflammatory “bad” eicosanoids (PGE2 series).
An even more powerful approach to preventing wrinkles is to increase the levels of “good” eicosanoids (PGE3 series) by increasing your intake of Omega 3 fatty acids. Due to their powerful anti-inflammatory actions, these good eicosanoids will do far more to reduce the inflammatory process that leads to wrinkles, than all the fruit acids and vitamin E creams you can possibly rub on your skin. This is because “good” eicosanoids are both very powerful vasodilators which increase blood flow to make your skin healthier. Increased blood therefore increases your production of the key structural proteins of the skin-collagen and elastin as you age. These structural proteins give your skin its firmness and elasticity. As the production of collagen and elastin decreases with aging, you skin starts to droop and sag. In order to keep collagen and elastin at increasing levels, you need to increase the blood flow to your skin, since that stimulates the enzymes that produce these structural proteins. With improved blood flow and decreased inflammation, you skin will look years younger.
Go to top of page.
Aids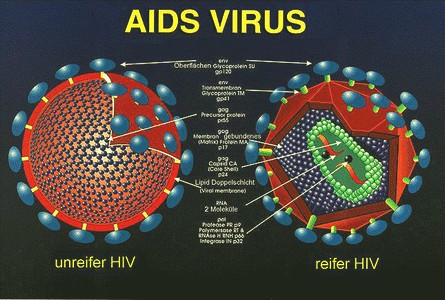
Aids (acquired immune-deficiency-syndrome) results from a shutdown of the immune system. Note that the name indicates that the condition is not genetic but acquired due to non-genetic (environmental) causes. Hence they should respond to environmental interventions that include changes in both nutrition and lifestyle. The consumption of Seal Oil and Omega 3’s per day along with a complete program of large doses of all other essential nutrients, many in supplement form, appear to be successfully prolonging survival. The exact mechanism of Seal Oil’s action is not yet clear but answers may be found in its ability to increase oxidation, increase peroxidation (which kills cancer cells and infectious microorganisms), develop cell membrane functions and form prostaglandins.
Go to top of page.
Allergies
Allergies are the bodies abnormal sensitivities to certain substances, a person can be allergic to just about anything i.e. dust, food, and medications etc. When our bodies are nutrient deficient, we need to replenish our bodies with a balance of Omega 3 and Omega 6’s, to increase the intake of good oils, Omega 3 and proteins.
Go to top of page.
Alzheimer’s
Docosahexaenoic acid (DHA), a major component of fish oils and seal oil, is the most important fatty acid in the brain and retina and makes up more than 30% of the structural lipid (fat) in neurons. There is ample evidence that a deficiency of DHA is associated with depression, attention deficit hyperactivity disorder, and dementia. Clinical studies have shown that an increased intake of DHA may benefit patients with dyslexia and Alzheimer’s disease.
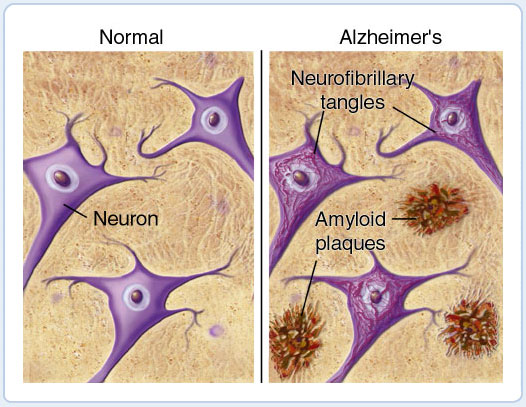 Researchers at Boston University and Tufts University School of Medicine now report that they have found a clear association between low blood levels (in the phosphatidylcholine fraction of serum) of DHA and the risk of developing Alzheimer’s disease. Their study involved 1188 elderly Americans (mean age of 75 years) who had blood samples drawn and analyzed for DHA in 1985. 16 of the participants were clinically diagnosed with Alzheimer’s at the time of blood sampling. The researchers noted that 11 of the 16 (69%) had lower DHA levels. The remaining 1172 participants were followed for 10 years. Again the researchers noted that participants with DHA levels in the lower half of the distribution had a 67% greater risk of developing Alzheimer’s disease.
Researchers at Boston University and Tufts University School of Medicine now report that they have found a clear association between low blood levels (in the phosphatidylcholine fraction of serum) of DHA and the risk of developing Alzheimer’s disease. Their study involved 1188 elderly Americans (mean age of 75 years) who had blood samples drawn and analyzed for DHA in 1985. 16 of the participants were clinically diagnosed with Alzheimer’s at the time of blood sampling. The researchers noted that 11 of the 16 (69%) had lower DHA levels. The remaining 1172 participants were followed for 10 years. Again the researchers noted that participants with DHA levels in the lower half of the distribution had a 67% greater risk of developing Alzheimer’s disease.
The researchers suggest that maintaining adequate levels of DHA through the consumption of fish oil, seal oil or dietary supplements rich in DHA may be particularly important for the elderly.
Go to top of page.
Angina
A team of British and Greek medical researchers report that fish oil supplementation is highly beneficial for angina patients.
METHODS: Their study involved 39 patients (37 men and 2 women) with stable angina pectoris who had experienced at least 6 angina attacks in the 2 weeks prior to the start of the trial. The patients were randomly assigned to receive either 10 grams of fish oil (providing 1.8 g eicosapentaenoic acid and 1.2 g docosahexaenoic acid) every day or 10 grams of olive oil daily. The daily supplements were supplied in the form of 5 identical looking capsules. The trial lasted for a total of 12 weeks and the patients were evaluated at baseline and after 8 and 12 weeks of supplementation.
RESULTS: By the end of the 12 weeks the number of weekly angina attacks had decreased by 41% in the fish oil group with no change observed in the olive oil group. The use of nitroglycerin (glycerol trinitrate) tablets decreased by 38% in the fish oil group and also decreased slightly (not statistically significant) in the olive oil group. Exercise tolerance, as measured on a treadmill, increased by 22.6% in the fish oil group, but no change was observed in the olive oil group. The blood level (fasting) of triglycerides decreased by 22% eight weeks into the test in the fish oil group, but then tended to approach pre-trial levels again by the 12th week. No statistically significant changes in blood coagulation parameters were observed in either group.
CONCLUSIONS: The researchers conclude that low-dose fish oil supplementation may benefit patients with coronary artery disease.
Go to top of page.
Arteriosclerosis (Artery Hardening)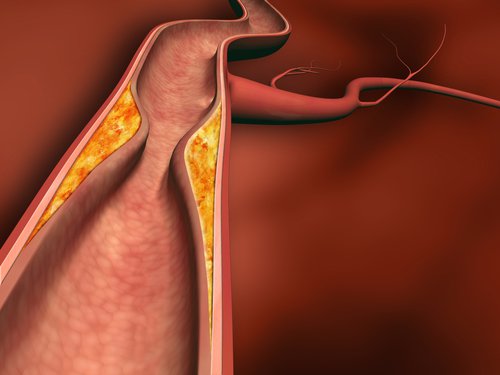
Dr.Garth Mulvad and Dr. Henning Pederson of the Department of Medicine, Dronning Ingrid’s Hospital in Norway recently wrote:
“…the International Arteriosclerosis Project… is a project supervised by experts at the Louisiana State University of New Orleans, USA. Among other things, they, “… studied the coronary arteries of the hearts of 23,000 deceased persons from 16 different countries. It is in the coronary arteries that the fatal blood clots form. The provisional results show that arteriosclerosis is far less widespread among the Inuit than elsewhere in the world…a seventy year old who has lived on the traditional diet of seal and whale has coronary arteries that are just as elastic as a twenty year old Dane.”
Go to top of page.
Arthritis
Long before it emerged as a possible remedy for heart disease, fish oil was used to treat arthritis. Maurice Stansby, veteran fish-oil researcher and scientific consultant to the National Marine Fisheries Service in Seattle, uncovered documents indicating that, in the late 1700’s, personnel from a hospital in Manchester, England, routinely dosed arthritis patients with cod-liver-oil supplements to help their “squeaky joints.” Stansby surmises that the fish-oil tradition was lost to history because it was so unpalatable – the only time patients would take their tonic was when it was forced upon them by attendants. No wonder, when cod-liver oil of the day was extracted from rotten fish livers!
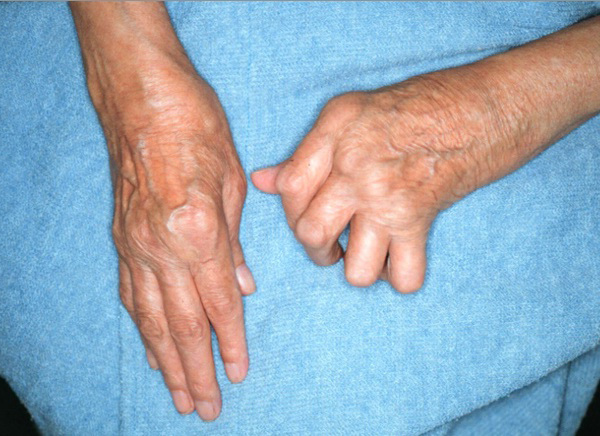 Interests in treating arthritis patients with fish oil, was rekindled by the finding that manipulating fatty acids in the diets of arthritic animals was beneficial. A link with fish oil was also suspected because of evidence that leukotrienes and thromboxane (a product of prostaglandins) are involved in the kinds of inflammatory reactions causing the painful symptoms of arthritis. Accordingly, Harvard researchers decided to test out the effects of fish oil in people who have rheumatoid arthritis, a form of arthritis that can be severely disabling. Richard Sperling, M.D., and his coworkers found a lowering of inflammatory biochemical, along with a decrease in joint pain and tenderness, in rheumatoid arthritis patients who took fish-oil supplements. Although the results are considered preliminary since no control group was involved, Dr. Sperling thinks that fish oils have the potential to act as anti-inflammatory drugs.
Interests in treating arthritis patients with fish oil, was rekindled by the finding that manipulating fatty acids in the diets of arthritic animals was beneficial. A link with fish oil was also suspected because of evidence that leukotrienes and thromboxane (a product of prostaglandins) are involved in the kinds of inflammatory reactions causing the painful symptoms of arthritis. Accordingly, Harvard researchers decided to test out the effects of fish oil in people who have rheumatoid arthritis, a form of arthritis that can be severely disabling. Richard Sperling, M.D., and his coworkers found a lowering of inflammatory biochemical, along with a decrease in joint pain and tenderness, in rheumatoid arthritis patients who took fish-oil supplements. Although the results are considered preliminary since no control group was involved, Dr. Sperling thinks that fish oils have the potential to act as anti-inflammatory drugs.
Support for Dr. Sperling’s hunch comes from research conducted at Albany Medical College in New York. Joel Kremer, M.D., found “modest” improvements in some symptoms of rheumatoid-arthritis patients who were on fish-oil capsules compared to a group of similar patients who did not take the supplements. The problem with this study is that the patients who took the capsules were also on a special diet, making it difficult to know whether fish oil or something about the diet was responsible. In a more recent study, Dr. Kremer placed people with rheumatoid arthritis on fish-oil supplements, but no special diet. Compared to a period of time in which they took a placebo (an inert supplement, often called a “sugar pill”), the fish-oil takers suffered significantly less joint tenderness and reported less fatigue. It’s important to note that, although there appeared to be overall improvement in other symptoms of arthritis such as duration of morning stiffness and joint swelling, the effects of fish-oil supplements were not as definite.
Thus, fish oil cannot be viewed as any sort of a panacea for arthritis sufferers. Furthermore, the small amount of research that has been conducted in this area has involved large amounts of fish oil. Dr. Dreamer’s patients, for example, took 10 to 15 fish oil capsules a day-surely a pharmaceutical dose. He issues words of caution when it comes to taking fish-oil supplements. But he does recommend that people who have arthritis eat more fish. At the very least a fish-rich diet can help keep weight down-an important move to minimize stress on weight-bearing arthritic joints.
Go to top of page.
Asthma
Anyone who struggles with asthma is all too familiar with the breathlessness, wheezing and coughing brought on by an attack. Since these aversive symptoms appear to be caused largely by leukotrienes, the search is on for remedies that will antagonize leukotriene synthesis. Enter another potential use for marine oil – in one study, large doses brought about the formation of less aggravating leukotrienes in asthmatics. But Walter C. Pickett, Ph.D., senior research biochemist at Lederle Laboratories in New York, who was involved in this research, notes that it is not yet known whether the change in leukotrienes helps alleviate asthma symptoms. One expert speculates that Eskimos may have a low incidence of asthma because they have hefty amounts of omega-3 fatty acids in their diets continuously from birth. Possibly, marine oils have an impact in the early stages of asthma – before asthmatics are sensitized to substances that bring on attacks. Dr. Pickett agrees it’s conceivable that eating fair amounts of fish starting early in life may influence the later development of asthma.
Go to top of page.
Atopic Dermatitis
An atopic disease is a form of allergy where the hypersensitivity reaction occurs at a location different from the initial contact point between the body and the offending agent (allergen). For example, food taken by mouth may cause an allergic skin reaction – atopic dermatitis. The incidence of atopic diseases such as dermatitis, allergic rhinitis, and asthma is rising in industrialized countries and now affects about 20% of the population.
A team of researchers from the University of Turku and Tufts University in Boston now report that the increase in atopic diseases is closely tied in with an increase in the consumption of omega-6 fatty acids (linoleic acid) which have pushed the ratio of omega-6 to omega-3 (alpha-linolenic, eicosapentaenoic, and docosahexaenoic acids) fatty acids in the diet to an unfavorably high level (10:1 or higher). An increasing dietary intake of linoleic acid has been linked to a rise in atopic diseases in both Germany and Japan. A recent study of Finnish and Swedish school children found that children with a high ratio of eicosapentaenoic acid to linoleic acid had a lower prevalence of atopic diseases while children with allergies tended to have a lower level of docosahexaenoic acid in their blood.
The researchers point out that the metabolic products (Eicosanoids) of omega-6 fatty acids promote inflammation while the metabolites of omega-3 acids dampens inflammation. They also point to several clinical trials, which have shown that supplementation with fish oil, or alpha-linolenic acid can reduce the symptoms of atopic dermatitis and asthma. They conclude that an increased intake of omega-3 fatty acids (fish oils and alpha-linolenic acid) may alleviate atopic diseases caused by an excessive intake of omega-6 fatty acids.
Go to top of page.
Attention Deficit Disorder
It is estimated that 3-5% of the school-age population in Canada and the United States suffer from attention-deficit hyperactivity disorder (ADHD). Prominent symptoms of this disorder are a poor attention span, inability to complete tasks, hyperactivity, and a tendency to interrupt others. Almost one quarter of children with ADHD also suffer from one or more specific learning disabilities in math, spelling or reading.
A study first reported in 1995-linked ADHD to a deficiency of certain long-chain fatty acids. These acids (arachidonic, eicosapentaenoic, and docosahexaenoic acids) are all metabolites of the two essential fatty acids, linoleic acid (omega-6) and alpha-linolenic acid (omega-3). Researchers at Purdue University are now leaning towards the conclusion that a sub clinical deficiency in docosahexaenoic acid (DHA) is responsible for the abnormal behavior of children with ADHD. They point out that supplementation with a long-chain omega-6 fatty acid (evening primrose oil) has been unsuccessful in ameliorating ADHD and believe this is because ADHD-children need more omega-3 acids rather than more omega-6 acids. The researchers also found that children with ADHD were breast fed less often as infants than were children without ADHD. Breast milk is an excellent source of DHA. A study is now underway to investigate the effect of oral supplementation with DHA on the behavior of ADHD-children.
Go to top of page.
 Autism
Autism
Previous studies link alteration in Omega 3 PUFA levels to psychiatric diseases, such as depression schizophrenia and attention deficit hyperactivity disorder (ADHD). Indeed, patients with schizophrenia or ADHD share poor communication skills and other behaviors with autism. For example polydipsia (excessive thirst) is a hallmark of autism, ADHD and essential fatty acid deficiency. On the other hand, Omega 3 PUFA levels differed markedly between autism and mentally retarded children. Levels of alpha-linolenic acid, the precursor for Omega 3 PUFA were not statistically different however DHA and total Omega 3 PUFA levels were 23 and 20 % lower respectively in autistic compared to mentally retarded children. Moreover the Omega 6/Omega 3 ratio increased by 25% among Autistic Children. Nevertheless the study offers the first evidence that children with autism show lipid abnormalities.
Go to top of page.
Autoimmune Diseases
Autoimmune disorders, in which the immune system begins attacking the body as if it were a foreign invader, can also be alleviated with marine oil Omega 3 fatty acid.
Multiple Sclerosis is one autoimmune disorder that can be positively affected by high-dose marine oil. Lupus, a life threatening autoimmune disorder that causes kidney failure, has also been shown to be positively affected by high doses of marine oil. In animal studies using rats that were bred to develop lupus, significant increases in their life spans are observed if their standard diet is supplemented by high dose marine oil.
IgA nephropathy is another inflammatory condition that attacks the kidneys. The disease, which is a major cause of kidney failure, has been found to be alleviated with marine oil. Long-term studies with marine oil indicate a dramatic reduction in the development of kidney failure in these patients compared with those taking placebo. Here, high-dose marine oil is acting not only as a modulator of eicosanoids, but likely also as an inhibitor of the release of various inflammatory cytokines.
Go to top of page.
Breast Cancer
Breast cancer rates differ greatly between countries. They are 5 times higher in the United States than in Japan and twice as high in France as in neighboring Spain.
Differences in overall fat consumption in these countries have been extensively studied, but no link to breast cancer incidence has been detected so far. A large team of researchers from the Netherlands, Ireland, Spain, Finland, Switzerland, Germany and the United States now report that, while overall fat consumption may not be significant, the make-up of the fats could be.
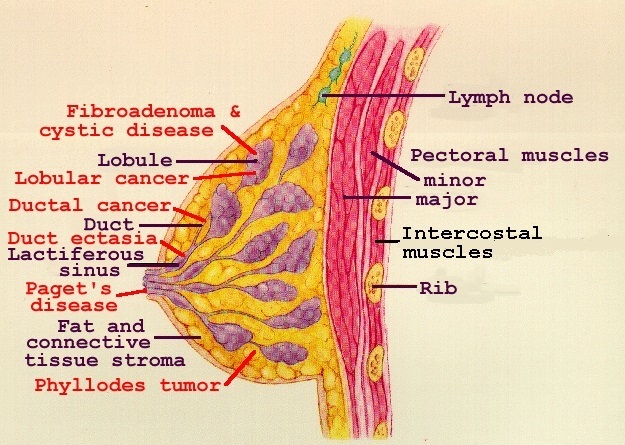 As part of the large EURAMIC Study the researchers investigated the link between the content of polyunsaturated fats in adipose (fat) tissue of postmenopausal women and breast cancer incidence. A total of 291 women with breast cancer and 351 controls were included in the study which involved 5 European medical centers. The women all had samples of adipose tissue taken (from the buttocks) and analyzed to determine the concentration of the main polyunsaturated fatty acids: the omega-3 acids – alpha-linolenic acid (ALA), eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), and the omega-6 acids – linoleic acid (LA) and its metabolite arachidonic acid (AA).
As part of the large EURAMIC Study the researchers investigated the link between the content of polyunsaturated fats in adipose (fat) tissue of postmenopausal women and breast cancer incidence. A total of 291 women with breast cancer and 351 controls were included in the study which involved 5 European medical centers. The women all had samples of adipose tissue taken (from the buttocks) and analyzed to determine the concentration of the main polyunsaturated fatty acids: the omega-3 acids – alpha-linolenic acid (ALA), eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), and the omega-6 acids – linoleic acid (LA) and its metabolite arachidonic acid (AA).
The study found no significant correlation between omega-3 fatty acid levels and breast cancer incidence, but did find a trend to higher incidences with increasing levels of omega-6 fatty acids in the adipose tissue samples. The researchers also found a significant association between the ratio of EPA and DHA to LA levels and breast cancer incidence in 4 out of 5 of the medical centers involved in the study. Pooling all results showed that women with the highest ratio had a 35% lower breast cancer incidence than women with the lowest ratio. In other words, women with a relatively high adipose tissue level of EPA and DHA (the main components of fish oils) and a relatively low level of LA and its metabolites had a lower breast cancer risk. The researchers note that LA (linoleic acid) is the precursor of certain eicosanoids which may promote tumour growth. EPA and DHA inhibit the production of these harmful compounds and may also, on their own, inhibit tumour growth. The researchers also point out that several epidemiological studies have found an inverse correlation between fish consumption and breast cancer incidence and urge further studies to determine the relationship between the dietary intake of specific fatty acids and breast cancer risk.
Go to top of page.
Cancer
Several major epidemiologic studies have found a clear association between a high dietary fat intake and the risk of developing breast and colon cancer. The correlation is particularly strong in the case of animal fats. One study found that a high fish or fish oil consumption is protective against later stage colon cancer in men but has no effect on mortality from breast cancer. British medical researchers now report that fish and fish oils not only protect against colon cancer in men, but also against colon and breast cancer in women. This protective effect, however, is only apparent in countries where the intake of animal fats is high. In other words, a high intake of fish or fish oils counteracts the detrimental effects of a high animal fat consumption.
The study compared cancer mortality rates in 24 European countries, Canada and the USA with fish consumption and the intake of animal fats. In countries where the animal fat intake was high the researchers found a clear inverse correlation between the ratio of fish fat to animal fat and the risk of developing breast cancer in women and colon cancer in both men and women. A similar correlation was found between cancer risk and the ratio of fish fat to total fat intake.
The researchers conclude that a 15% decrease in animal fat intake combined with a 3-fold increase in fish oil intake could possibly reduce male colon cancer risk by as much as 30% in countries with a high animal fat intake. A 3-fold increase in fish oil intake could be achieved by eating fish three times a week or by taking two standard fish oil capsules daily.
Studies indicate the following:
Feeding omega 3 has slowed the growth of the tumour and made it less likely that the cancer would spread.
– Galli, Claudia, Butrum, Simopoulos et al, eds 1991, Karger, Basel, p462-476
A study of 12, 866 American men determined that those eating high amounts of omega 3 and low amounts of omega 6 had a 33% lower risk of dying from cancer.
– Dolecek, There and Grandits, World Review Nutr. Diet, Karger, 1991, 66: 205-216
Tissues taken from 100 skin cancer patients were compared with skin from 100 healthy individuals and it was found that the more omega 6 found in a person’s tissues, the more likely they were to have cancer.
– MacKie, MacKie and Bourne, Nutr and Cancer, 1987 9, 205-216
A comparison of cancerous brain tumours with healthy tissue revealed that omega 6 was 4x more prevalent in the cancerous tissues.
– Martin, Robbins and Hussy, Lipids, 1996, 31: 1238-1288
Incidence of breast cancer increased as Greenland and Icelandic women abandoned their traditional diets of marine life (mainly seal which is very high in omega 3)
– Bjarnason, Int. J., Cancer, 1974, 13: 689-696
In a 8 year study of 846 men, those given a diet high in omega 6 were twice as likely to die of cancer as those eating a diet low in omega 6.
– Pearce and Dayton, The Lancet, 1971, 464-467.
“For breast cancer, omega 6 fatty acids appear to have the greater cancer promoting effects and omega 3 fatty acids are the most protective.”
- L. Williams, M., Bollella, Laura Boccia and Arlene Spark, “Dietary Fat and Children”
- Nutrition today, vol 33, no 4: July/Aug 1998
In animal experiments, dietary corn oil very high in omega 6 has been shown to stimulate lung cancer of the adenocarcinoma type.
– Okuyama, Kobayashi and Watanabe. p.415
How does Omega 3 Reduce Cancer or the Risk Of Cancer?
Research indicates the following: Consuming more omega 3s make the omega 6 linolenic acid that promote tumor growth less available. Omega 3 makes the cancer cells more vulnerable to free-radical attack by rendering the membranes less saturated. Omega 3 seems to promote the self-destruction of cancer cells thereby slowing tumor growth.
Go to top of page.
Cardiovascular Disorders
The International Arteriosclerosis Project (1992)
Since 1990, researchers from the Louisiana State University have analyzed the coronary arteries of 23,000 deceased persons from 16 countries. The interim results reveal that the Greenlanders have the lowest rate of arteriosclerosis among all those tested.
Some of the fascinating early results are as follows:
1) The Inuit who ate a modern diet had the same rate of this disease as ordinary Europeans and therefore the results were not based on heredity.
2) The Inuit who lived on a traditional diet of marine mammals (mainly seal) had, at the age of seventy, the same coronary artery elasticity as a 20 year old European.
3) Some European countries may eat more fish than is found in the traditional Greenland diet, but have a far higher incidence of arteriosclerosis and, in general, higher levels of cholesterol.
At the National Hospital in Nuuk, a person with very high cholesterol was given various diets and medicines without major impact. When he was placed on a traditional Greenland diet (mostly of seal) his cholesterol level fell dramatically in one month.
The Orsoq Study
Dr. E. Jorgenson of the Center of Arctic Environmental Medicine in Denmark recently presented the initial results of the Orsoq Seal Research Project, a pilot study on the effect of seal oil on human health. These preliminary findings indicate that the general population of Denmark, fed on a modern diet, was ten times more likely to develop cardiovascular and inflammatory diseases that Greenlanders on their traditional diet of seal, a food high in omega 3
“Inuit Whaling”, Inuit Circumpolar Conference, June 1992, special issue. Gerth Mulved and Henning Sloth Pederson, Doctors of Medicine Dronning Ingrids Hospital
Numerous studies show that increased long term intake of marine oils, rich in EPA and DHA, reduces the morbidity and mortality associated with cardiovascular disorders in middle-aged men. Conflicting data exist as to whether it is EPA or DHA, or the combination which is responsible for the various beneficial effects. In any event, it is known that there may be limits to the elongation and desaturation of EPA to DHA, whereas the retroconversion of DHA to EPA occurs.
– Harris et al., Grimsgaard et al., 1995
It is generally agreed that omega-3 fatty acids moderate hyperlipidemia – particularly hypertriglyceridemia, very rapidly in a dose dependent manner. Omega-3 fatty acids reduce the triglyceride levels in the blood by a reduced synthesis and secretion of VLDL particles from the liver and enhances the in vivo lipolysis of the VLDL-particles. An improved balance between LDL-cholesterol and HDL-cholesterol is also normally found, whereas the effect on total cholesterol is marginal. A large number of studies report such findings. Omega-3 fatty acids influence on platelet aggregability at rather low doses (50-350mg), whereas significant effects on blood lipids and blood pressure can be achieved at higher doses (2 g/day).
– Christensen et al, 1995
Recent data (from a parallel group study) show that 3g pure DHA (95% DHA, ethyl ester) produce a 30-40% greater reduction in triglyceride levels in plasma than a corresponding amount of EPA (90% EPA, ethyl ester). DHA also seems to have a more marked effect on increasing HDL-cholesterol, whereas EPA was found to slightly decrease both total cholesterol and APO-1 in normal subjects
– Grimsgaard et al, 1995
This study suggests that DHA might be more beneficial than EPA in terms of effects on blood lipids. Others have reported that DHA-rich oils (4g/day, 42% DHA) are less active than EPA-rich oils and fish diet on both fasting and postprandial triglyceride levels.
– Argen, 1995
A positive correlation has been observed between supplementation with EPA and DHA (85% ethyl ester) and improvements in blood pressure and heart rate in subjects suffering from mild hypertension. Recently published studies showed that DHA (EE), not EPA (EE), lowered the heart rate in healthy humans.
– Bönaa el al, 1995
Even short time supplementation with large amounts (19g/day) of a combination of EPA and DHA (as ethyl esters) has shown to have long-lasting effects on the human platelet aggregation, an effect suggested by inhibition on TXA2/PGH2 receptor by EPA and/or DHA-sensitive mechanisms.
– Di Minno et al,1995
Studies on cardiac arrhythmias do not give any clear evidence on the efficacy of omega-3 fatty acids. However, a trend towards reduction in ventricular extracystoles in patients with ventricular tachyarrhythmias has been observed after supplementation with omega-3 fatty acids
-Christiansen et al,1995
Animal studies show that DHA may inhibit ventricular tachyarrhytmias more significantly than EPA
– Leaf, 1995
and also increases the cardiac contractibility.
– Grynberg et al, 1995
Recent data also show that DHA has more pronounced inhibitory effect on the expression of cytokines in endothelial cells, which clearly downregulate the inflammatory process and may inhibit the progression of arteriosclerosis.
– DeCaterina & Libby, 1995
Epidemiological and clinical research have shown that omega-3 fatty acids intervene in the arteriosclerotic process at all steps, and that there probably are synergistic effects of EPA and DHA at many levels.
– Argen,1995
Go to top of page.
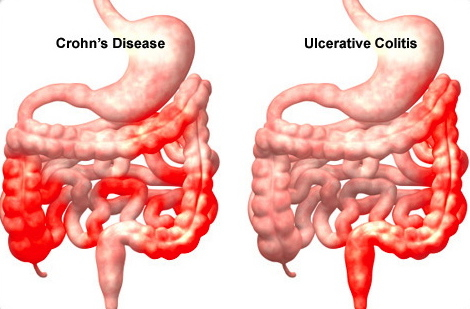 Crohn’s Disease
Crohn’s Disease
Crohn’s disease is an inflammatory disease involving intestinal pain, diarrhea, and malabsorption of nutrients. The disease is characterized by periods of active disease interspersed with periods of remission. Elemental diet (ED) therapy is the preferred treatment in Japan. Conventional treatment with prednisone and salycylates has been only marginally successful in extending the periods of remission. The ED therapy involves tube feeding (enteral nutrition) a mixture of free amino acids, short-chain maltodextrins, and low levels of fat in the form of soybean oil. Not surprisingly, compliance with this diet is poor resulting in shorter periods of remission.
Researchers at the University of Bologna report that fish oils can prevent relapses. Their experiment involved 78 patients with Crohn’s disease who had been classified as having a high risk of relapse. Half the patients were randomized to receive nine fish oil capsules daily, the other half received nine placebo capsules daily. The fish oil capsules contained 500 mg of a marine lipid concentrate each (40 per cent eicosapentaenoic acid and 20 per cent docosahexaenoic acid) and provided a total of 2.7 grams of n-3 fatty acids per day. The capsules were enteric-coated so as to ensure that they dissolved in the small intestine instead of in the stomach and to minimize unpleasant side effects such as flatulence, heartburn, belching, and diarrhea. The results of the fish oil therapy were spectacular. While 69% of the patients in the control group had a relapse during the one-year study period, only 28% in the therapy group did. At the end of the one-year period 59% of the patients in the fish oil group were still in remission as compared to only 26% in the placebo group. The researchers conclude that fish oil therapy (with enteric-coated capsules) is effective in preventing relapses in patients with Crohn’s disease in remission.
Go to top of page.
Cystic Fibrosis
Seriously ill Cystic Fibrosis (CF) patients cannot absorb fats and other nutrients properly and therefore often need infusions of essential fatty acids. These infusions are most often based on linoleic acid as many CF patients have been found to have a deficiency of this omega-6 fatty acid. There is now substantial evidence that long-chain omega-3 fatty acids found in fish oils can suppress inflammatory processes such as those involved in CF.
A team of American, Finnish, and German researchers completed a small clinical trial aimed at determining if it would be safe and effective to use a fish oil fortified emulsion in the intravenous feeding of CF patients. The trial involved 12 patients; 6 were given infusions of a lipid emulsion enriched with fish oils while the remaining 6 (control group) were given infusions of the standard linoleic acid-based emulsion. The fish oil emulsion contained 18.3% eicosapentaenoic acid (EPA), 27.6% docosahexaenoic acid (DHA), 12.7% oleic acid, and 2.5% linoleic acid. The standard emulsion contained 54.5% linoleic acid, 22.4% oleic acid, and 0% EPA and DHA. Both emulsions were administered daily (over a 4-hour period) for 1 month at a dose of 150 mg/kg of body weight. The researchers found no adverse effects on liver function or coagulation parameters and no toxic or allergic reactions in the patients receiving the fish oil emulsion. There was a tendency to improved lung function in the fish oil group and a tendency towards a worsening in the control group during the trial; however, these effects were not statistically significant.
The researchers conclude that intravenous infusions of lipid emulsions containing fish oils are safe for CF patients. They urge additional, longer-term studies to determine if such infusions would be of clinical benefit.
Go to top of page.
 Depression
Depression
Researchers at the National Institute of Alcohol Abuse and Alcoholism believe that the increasing rates of depression seen in North America over the last 100 years are due to a significant shift in the ratio of n-6 (arachidonic acid, linoleic acid) to n-3 (docosahexaenoic acid, linolenic acid) fatty acids in the diet. The human race evolved on a diet having a ratio of about 1:1 of these acids; it is now estimated to be between 10:1 and 25:1. Docosahexaenoic acid (DHA) is a main component of the synaptic membranes and a lack of it has been linked to depression. Fish oils are a rich source of DHA and it can also be biosynthesized in the body from linolenic acid.
The researchers speculate that the depressions which often accompany alcoholism, multiple sclerosis, and childbirth (postpartum depression) are all due to a lack of DHA and can be corrected by increasing the dietary intake of DHA or linolenic acid (seal oil). They also point out that depression and coronary heart disease are strongly associated and that a low intake of n-3 fatty acids has been linked to both.
Cornell University
The relation of omega-3s — principally DHA and EPA (eicosapentaenoic acid) — and depression has been revealed in several studies worldwide. In a large Finnish study of fish consumption and depressive symptoms, published in Psychiatric Services in April 2001, Tanskanen, et al. demonstrated that the likelihood of having depressive symptoms was significantly higher among infrequent fish consumers than among frequent fish consumers. They theorized that the human brain is adapted to Paleolithic diets of our ancient ancestors, whose diet comprised equal proportions of omega-3 fatty acids and omega-6 fats (found in corn and soy seed oils). In the past 100 years, Western diets have lowered the ratio of omega-3 to omega-6 to about 1:25; simultaneously, the prevalence of major depression has increased.
In the 2003 Rotterdam Study, published in the American Journal of Clinical Nutrition, Tiemeir, et al. found that elderly persons with depression had a fatty acid composition different from that of non-depressed persons. Percentages of omega-3 polyunsaturated fatty acids (PUFAs) were significantly lower, and the ratios of omega-6 to omega-3 PUFAs were significantly higher in subjects with depressive disorders than in control subjects.
Dr. Joseph R. Hibbeln of the National Institute on Alcohol Abuse and Alcoholism, part of the National Institutes of Health (NIH), discovered that omega-3 may influence serotonin functionality in the brain. In a letter published in The Lancet in April 1998, he reported that among healthy volunteers, low plasma concentrations of DHA predict low concentrations of a marker of brain serotonin turnover. Low concentrations of serotonin are strongly associated with depression and suicide.
DHA is a primary building block in the gray matter of the human brain and in the retina of the eye, and is present in every cell in the body. It is essential at every stage of human life, beginning in utero. DHA, like EPA, must be derived from foods because the body cannot produce its own supply. It is available in fish and as a pure pharmaceutical-grade nutritional supplement, with an ideal ratio of omega-3s to omega-6s (10:1). Source: Cornell University
Go to top of page.
Diabetes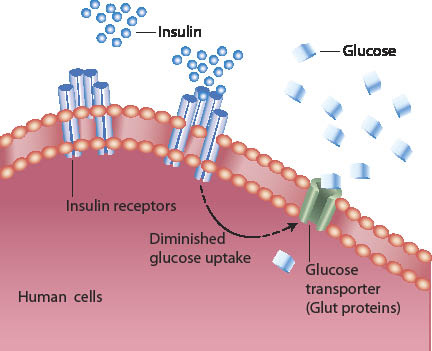
Diabetes is a disorder characterized by high blood levels of glucose in the blood. Diabetes can damage the large blood vessels increasing the risk of stroke, heart attack, and in the limbs, can lead to gangrene. Many studies now suggest that omega-3 is invaluable in combating circulation problems associated with diabetes by rendering the walls of the veins and arteries smoother and more elastic.
In another study published in 1994 by the British Nutrition Foundation they reported that daily consumption of seal oil (high in omega 3), by Alaskan natives led to a 20% lowering of glucose intolerance and diabetes.
– Adler, Boyko, Schraer, Murphy, 1994 Nutrition Supplement
A recent study published by Tokyo Medical and Dental University, indicates that the DPA component of the omega 3 can be more than TEN TIMES AS EFFECTIVE as EPA in helping to heal damaged blood vessels, seal oil is the ONLY supplement rich in natural DPA.
Go to top of page.
Dyslexia
Dyslexia is a fairly common condition, which involves difficulties in learning to read and write, mirror reversals of letters and words, and poor short-term memory. Dyslexia is closely related to dysphasia (problems with coordination and muscle control) and attention-deficit hyperactivity disorder. It is estimated that about 10% of the populations of the United States and the United Kingdom suffer from dyslexia and 4% are severely affected. There was a 3-fold increase in the prevalence of learning disorders in the USA over the period 1976 to 1993 and 80% of the new cases involved dyslexia.
Dr. Jacqueline Stordy of the University of Surrey believes that dyslexia, dyspraxia, and attention-deficit hyperactivity disorder have one common denominator – a deficiency of long-chain fatty acids. She points to a study which found improved dark adaptation (a problem among dyslexics) after supplementation with 480 mg/day of docosahexaenoic acid (a main constituent of fish oil) for a month. Another study involving 15 dysphasic children found that supplementation with a proprietary mixture of tuna oil, evening primrose oil, thyme oil, and vitamin E for 4 months markedly improved their motor skills. The mixture provided 480 mg of docosahexaenoic acid, 35 mg of arachidonic acid, 96 mg of alpha-linolenic acid, 80 mg of vitamin E, and 24 mg of thyme oil daily. Dr. Stordy concludes that long-chain polyunsaturated fatty acid supplements may benefit children with dyslexia, dyspraxia, and attention-deficit hyperactivity disorder and notes that large, double-blind, placebo-controlled studies are already underway to verify this hypothesis.
Go to top of page.
Dysmenorrhea (Menstrual Cramping)
Fish oil supplements particularly if they also include Vitamin B12 can alleviate menstrual discomfort in young women. Menstrual pain is generally attributed to prostaglandins. (PG) hence the efficiency of NSAIDS, which inhibits their synthesis. However the PG’s most likely to blame are those derived from Omega -6 LC PUFA. Rather than those of the Omega-3 Series, which are less biologically active. Indeed there is evidence that levels of dietary Omega-3 LC PUFA are lower in women with, than without dysmenorrhea. Fish oil plus vitamin B12 should be superior to fish oil alone. Possibly the vitamin is involved in the prostaglandin metabolism or has antioxidant effects. They conclude that the supplementations with Omega-3 LC PUFA and vitamin B12 may server as an alternate treatment to NSAID medication against Dysmenorrhea in young women. Two important advantages are, combination appears to be essentially without adverse effects, and it is easy to administer.
Go to top of page.
Eczema
Eczema is a skin disease, especially conditions that cause dry scaly skin like eczema often result from excessive levels of ‘bad’ eicosanoids (Omega-6 PGE 2 series). While eczema is not life threatening, it is a cause of concern because it indicates that a significant inflammatory process is already taking place in the skin. Research shows eczema stems from the overproduction of ‘bad’ eicosanoids called leukotrienes. Reducing Arachidonic acid levels by using high dose marine oil chokes off the production of leukotrienes, while simultaneously increasing the levels of ‘good’ eicosanoids.
Dermatologists usually prescribe corticosteroid creams to reduce inflammation, but these drugs unfortunately knock out ‘good and bad’ eicosanoids and that leads to a thinning of the skin. Various studies have indicated that high dose marine oil, without the use of corticosteroid, can contribute to some improvement in eczema.
Go to top of page.
Fatty Liver
Fatty liver in patients is most commonly found in the early stages of cirrhosis of the liver with or without excessive alcohol involvement. Fatty liver is also commonly associated with liver pathologies and metabolic disturbances with obesity, diabetes, hyperlipidemia, and exposure to certain toxins.
Fatty liver is defined as lipid infiltration in more than 50% of hepatocytes mainly in the form of big lipid droplets. In patients with fatty liver, recent clinical research has found that the concentration of the long chain Omega 3 fatty acid is very low. Also, research has found that an increase in fat droplet size in hepatocytes is associated with a decrease of the percentage of Omega 3 in the liver triglycerides.
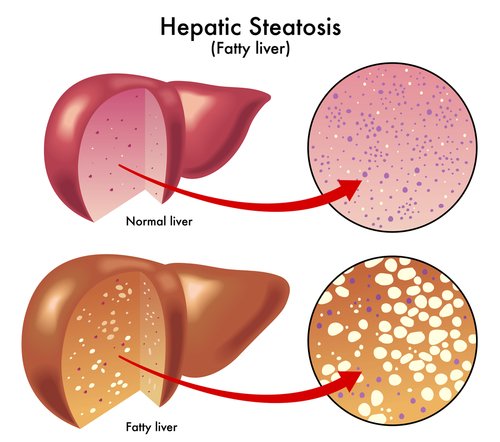 The most common cause of fatty liver today is chronic alcoholism, where the alcohol damages liver cells and causes malfunction of the liver metabolism. This in turn causes lipid, carbohydrates and protein metallic disturbances. Overeating increase lipid carbohydrates and protein intake compound this. Most commonly this patient will develop obesity, hyperlipidemia, insulin resistance, hypertension and visceral distribution of the adipose tissue.
The most common cause of fatty liver today is chronic alcoholism, where the alcohol damages liver cells and causes malfunction of the liver metabolism. This in turn causes lipid, carbohydrates and protein metallic disturbances. Overeating increase lipid carbohydrates and protein intake compound this. Most commonly this patient will develop obesity, hyperlipidemia, insulin resistance, hypertension and visceral distribution of the adipose tissue.
Recent clinical findings have found patients with end-stage liver disease manifest a wide variety of functional abnormalities that eventually lead to their deaths. Such patients also have low levels of polyunsaturated fatty acids (PUFA) of carbon lengths 20 or greater in plasma. (C20:5W-3 EPA, C22:5W-3 DPA, C22:6W-3 DHA). This is due to hepatic damage and impairment of the 20-22 carbon PUFA from their fatty acids 18 (alpha linolenic acid) carbon dietary precursors. This normally takes place principally in the liver.
Long chain Omega 3 fatty acids have been proven to decrease the LDL cholesterol (low density lipoprotein), serum triglycerides, platelet aggregability, blood viscosity, hypertension, glycerolipid synthesis, and reduce the fatty droplet deposit to the liver. These fatty acids have also been shown to improve the insulin resistance, liver function, and enhance red cell deformability. In addition, they alter the cellular membrane phospholipids Omega 3 fatty acid concentration, which increases the cellular metabolic rate as well as cellular functions. Therefore, directly and indirectly Omega 3 long chain polyunsaturated fatty acids (Seal Oil) improves the general condition of the liver and can effectively treat or even prevent the occurrence of fatty liver. Because fatty liver is a malfunction of the liver as well as a disturbance of metabolism of fat, protein and carbohydrates overeating and overindulgence of alcohol should be eliminated.
Go to top of page.
Fibromyalgia
Post Viral Fatigue CFIDS (chronic fatigue and immune dysfunction syndrome) is an illness characterized by a number of symptoms rather like a severe flu. It affects the body and the mind. It is also known as post viral fatigue syndrome (PVFS) and Fibromyalgia. It has probably been in existence for many years, but it is poorly understood and has been called by different names at different times.
The characteristic features are fatigue, which goes on for more than 6 months and for which no other cause can be found. It may follow an infection like flu or tonsillitis. The fatigue affects both mental and physical activity and is not relieved by rest. Other symptoms may include sweating, shivering, feeling cold, headaches and nausea. Bowel problems such as diarrhea or constipation can occur. Visual problems and generalized aches and pains especially in muscles or joints may occur. Patients complain of poor memory and difficulty in concentrating.
All these symptoms may vary from day to day and are often made worse by minimal physical or mental effort. Mood swings may occur and people may feel tearful and depressed. Patients become particularly frustrated that no clear explanation for their illness can be found. They are also somewhat characteristically “high achievers” who were more energetic than average prior to becoming ill.

Go to top of page.
Heart Disease
Heart disease remains the leading cause of death in western society. For men, the risk of heart attack begins very young and remains fairly constant throughout life while the female incidence of heart disease begins to equal and surpass that of men as women reach menopause. Studies indicate that omega 3 can reduce the chance of a primary cardiac arrest by 70% and a second arrest by 30% This results primarily from the fact that omega 3 facilitates the maintenance of the walls of the blood vessels, making them smoother and more elastic, thus reducing vessel blockages which are often the cause of heart problems.
Omega 3 also tends to retard the rate of the blood clotting, by reducing the “stickiness” of platelets. Heart muscle damage may still take place from a temporary stoppage of an artery, and omega 3 PUFAs prevent this damage from interfering with heartbeats.
Studies further indicate that omega 3 helps reduce a person’s blood pressure, which is becoming a chronic problem in an aging population.
Go to top of page.
High Blood Pressure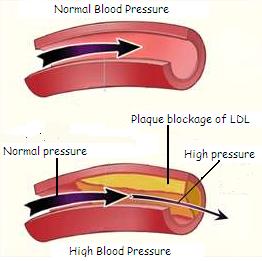
Go to top of page.
Hyperactivity (ADHD)
Children suffering from attention-deficit hyperactivity disorder (ADHD) are inattentive, impulsive, and hyperactive. Researchers at Purdue University now report that hyperactive children have lower levels of key fatty acids in their blood than do normal children. Their experiment involved 53 boys aged 6 to 12 years of age who suffered from ADHD, but were otherwise healthy and 43 matched controls. Analyses showed that the boys with ADHD had significantly lower levels of arachidonic, eicosapentaenoic, and docosahexaenoic acids in their blood.
The hyperactive children suffered more from symptoms associated with essential fatty acid deficiency (thirst, frequent urination, and dry hair and skin) and were also much more likely to have asthma and to have had many ear infections. The researchers conclude that ADHD may be linked to a low intake of omega-3 fatty acids (linolenic, eicosapentaenoic, and docosahexaenoic acids) or a poorer ability to convert 18-carbon fatty acids to longer more highly unsaturated acids. The researchers conclude that supplementation with the missing fatty acids may be a useful treatment for hyperactivity.
Go to top of page.
Kidney Disease
A newly reported clinical trial has strengthened the argument for recommending daily treatment with n-3 polyunsaturated fatty acids in patients with immunoglobulin A nephropathy (the most common form of primary glomerulonephritis in the world) who are at high risk for progression of renal disease. Studies are underway that involve a combination of cyclosporine A, a commonly prescribed immunosuppressive agent in solid-organ transplantation, with a high-potency n-3 polyunsaturated fatty acid to reduce cyclosporine toxicity. Studies reported during the past year show promise that dietary supplementation with n-3 polyunsaturated fatty acids will substantially decrease vascular access graft thrombosis in patients receiving maintenance hemodialysis, and may reduce hypercalciuria in patients who suffer from kidney stones.
Go to top of page.
Learning Disorder
Children suffering from attention-deficit hyperactivity disorder (ADHD) are inattentive, impulsive, and hyperactive. Researchers at Purdue University now report that hyperactive children have lower levels of key fatty acids in their blood than do normal children. Their experiment involved 53 boys aged 6 to 12 years of age who suffered from ADHD, but were otherwise healthy and 43 matched controls. Analyses showed that the boys with ADHD had significantly lower levels of arachidonic, eicosapentaenoic, and docosahexaenoic acids in their blood. The hyperactive children suffered more from symptoms associated with essential fatty acid deficiency (thirst, frequent urination, and dry hair and skin) and were also much more likely to have asthma and to have had many ear infections. The researchers conclude that ADHD may be linked to a low intake of omega-3 fatty acids (linolenic, eicosapentaenoic, and docosahexaenoic acids) or a poorer ability to convert 18-carbon fatty acids to longer more highly unsaturated acids. The researchers conclude that supplementation with the missing fatty acids may be a useful treatment for hyperactivity.
Go to top of page.
Ligament Injuries
Ligaments are tough bands of fibrous connective tissue (mainly collagen) that link two bones together at a joint. Injuries to ligaments are notoriously slow to heal. Researchers at Purdue University now report the results of an intriguing experiment which shows that eicosapentaenoic acid (the main component of fish tissue oils) maternally speeds up the healing of ‘wounded’ ligament cells in vitro. The researchers conclude that dietary supplements with marine oils (n-3 polyunsaturated fatty acids)could be used to improve the healing of ligament injuries by enhancing the entry of new cells into the wound area by speeding up collagen synthesis.
Go to top of page.
Lupus
Lupus is an immune disorder that can ravage the body; attack organs from kidneys to brain. Supplements of Omega 3 fatty acids have reduced inflammation, kidney problems and mortality. In one-study patients with active lupus showed significant improvements on supplements of Omega-3 oils. While it may be unlikely that most patients with lupus could replace their conventional anti inflammatory drugs with Omega-3 Fatty Acids there may be a place for using the Omega 3’s as adjuncts.
Go to top of page.
Macular Degeneration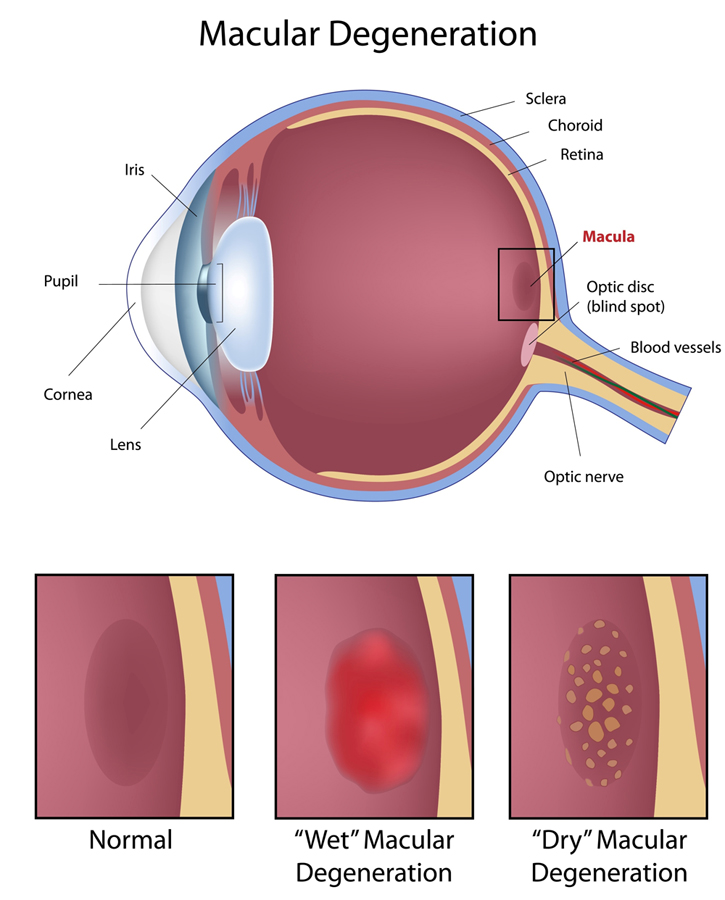
Age-related macular degeneration (AMD) is a leading cause of blindness for which treatment options are limited. The macula is responsible for detailed, fine central vision and is located at the center of the retina. Researchers at the Harvard medical school have just released a major study that points to a close association between the development of AMD and the consumption of certain fats. The major contributors to the increased risk were high intake of linolenic acid and trans fatty acids with a 35 percent increased risk of AMD. In contrast, a high intake of docsahexaenoic acid (DHA), a main component of marine oils was found to lower the risk of AMD by about 30 percent.
Go to top of page.
Menopause
During menopause your ovarian function starts to decline, reducing your bodies production of estrogen by about two-thirds (your adrenal glands and fat cells make the remaining amount). During this time of rapid hormonal changes, your body’s eicosanoids balance gets thrown off, giving rise to hot flashes and other discomforts. New evidence suggests that hot flashes may stem rapidly changing levels of eicosanoids and may be due in part to overproduction of the ‘bad’ eicosanoids PGE 2 series. One reason may be that the plunge in estrogen levels during menopause also leads to a corresponding increase in the production of insulin. The increase in insulin leads to increased production of Arachidonic acid, the building block of ‘bad’ eicosanoids such as the PGE 2 series. High doses of marine oil (omega 3 fatty acids) will reduce the production of eicosanoids by lowering the level of Arachidonic acid.
Moreover, Japanese and Chinese woman who consume large amounts of seafood and soy rarely suffer from hot flashes. Researchers have found that eating 20 grams of soy protein (which is rich in a chemical called phytoestrogens) per day provides a modest decrease in the variety of menopausal symptoms. However, phytoestrogens are not the cure all that they were hoped to be, because without adequate levels of long chain Omega 3 fatty acids, there would not be the full inhibition of excess PGE 2 Series production.
Go to top of page.
Mental Illness
Researchers at the National Institute of Alcohol Abuse and Alcoholism believe that the increasing rates of depression seen in North America over the last 100 years are due to a significant shift in the ratio of n-6 (arachidonic acid, linoleic acid) to n-3 (docosahexaenoic acid, linolenic acid) fatty acids in the diet. The human race evolved on a diet having a ratio of about 1:1 of these acids; it is now estimated to be between 10:1 and 25:1. Docosahexaenoic acid (DHA) is a main component of the synaptic membranes and a lack of it has been linked to depression.
Seal oils are a rich source of DHA and it can also be biosynthesized in the body from linolenic acid. The researchers speculate that the depressions which often accompany alcoholism, multiple sclerosis, and childbirth (postpartum depression) are all due to a lack of DHA and can be corrected by increasing the dietary intake of DHA or linolenic acid.
They also point out that depression and coronary heart disease are strongly associated and that a low intake of n-3 fatty acids has been linked to both.
Go to top of page.
Multiple Sclerosis
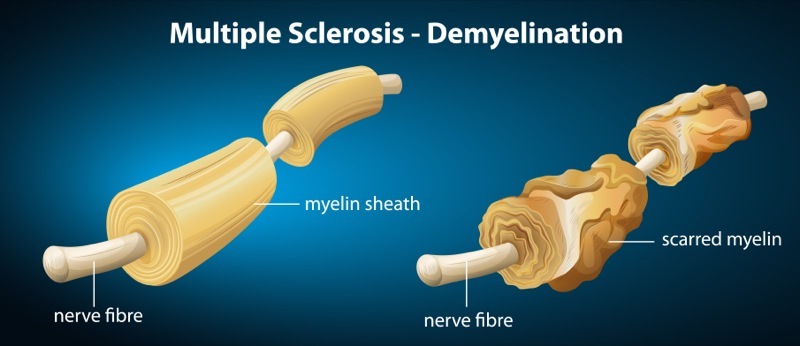
Multiple Sclerosis is a disease, which leaves the patient in an unresponsive body but with mental functions intact. With Multiple Sclerosis, the insulating membrane that coats the nerve cells unravels, making it difficult for the nerve cells to transmit their signals. Although the molecular cause of multiple sclerosis is unknown, scientists have learned that it is primarily driven by inflammation.
Multiple Sclerosis is virtually unknown amongst the Eskimos of Greenland. Their high intake of long chain Omega 3 fatty acids provides a clue to the prevention and treatment of this condition like all inflammatory conditions, multiple sclerosis characterized by overproduction of ‘bad’ eicosanoids.
Long chain Omega 3 fatty acids are anti-inflammatory agents that can cross the blood-brain barrier. Patients with Multiple Sclerosis are known to have low levels of DHA in the brain. It is also known that long chain Omega 3 fatty acids inhibit the production of pro-inflammatory cytokines like gamma interferon, similar effects that are behind the theory of constant injections with beta-interferon. This may explain why populations that consume the most fish have the lowest rates of multiple sclerosis.
Go to top of page.
Obesity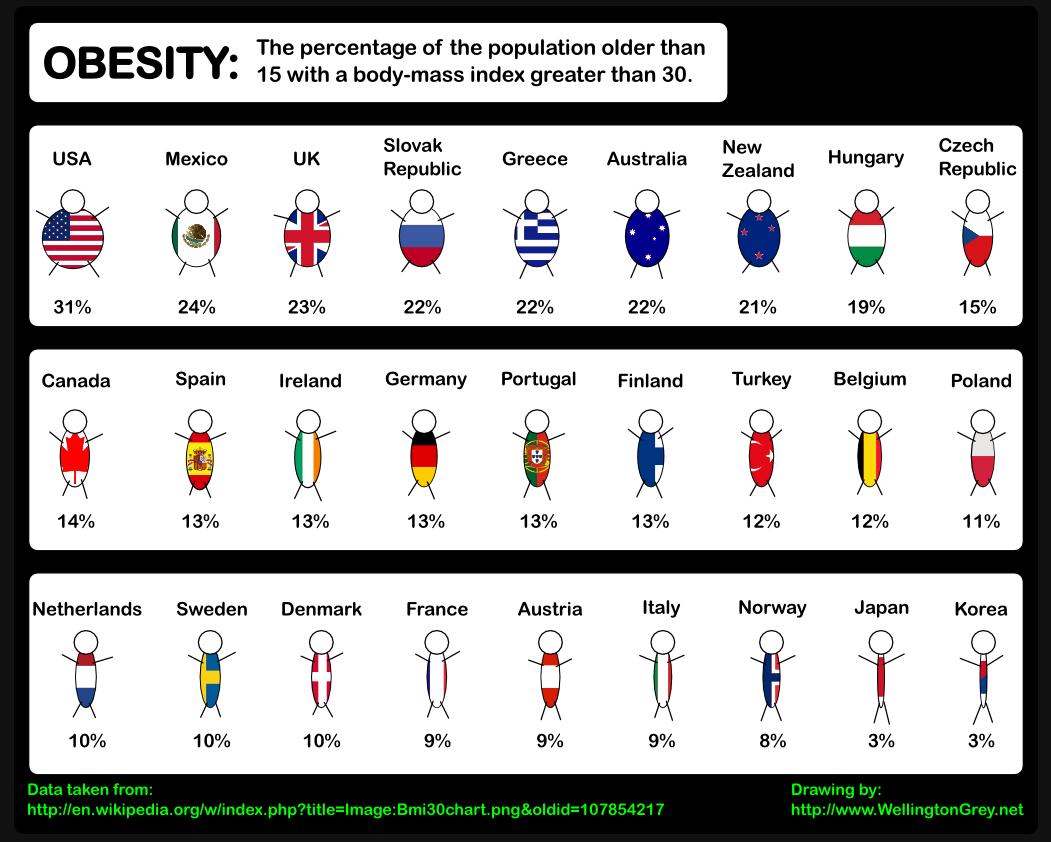
Omega 3 fatty acids which increase metabolic rates, can be used for weight loss. The right kind of fat can actually help you with losing weight. Omega 3 serves as building materials for series 3 prostaglandin, some of which help our kidneys get rid of excess water held in tissues. The excess weight of some overweight people is largely retained water (edema). Omega 3 helps to dump this water. Omega 3 increase metabolic rate, oxidation rate, and energy production. This effect begins to show up when 3 or more tablespoons of Omega 3 (5 capsules) per day are used. When metabolic rate goes up, more fat and glucose are burned. Less fat deposition takes place.
This increased production of energy is the opposite of what happens when we fast or diet, on calorie- restricted programs. The latter decrease our metabolic rate, and lead us to put on weight even on a small intake of food. There is evidence that obesity is the result of gross over eating in only 10% of cases. The other 90% are lacking exercise and choosing foods lacking important essential nutrients. Omega 3 helps us to lose weight and increase our energy levels, with the end result being more energetic. This is a special bonus, because activity makes us feel good, builds lean body (muscle) mass, makes us healthier, increases our metabolic rate and resets our fat thermostat to a lover level, helping make weight loss permanent.
Go to top of page.
Pregnancy
According to Crawford (1995), the first pregnancy-related need for PUFAs (both omega-6 and omega-3) occurs during the three months prior to conception. This critical period for cell commitment and division requires ARA and DHA to facilitate growth and development. It has been suggested that supplementation with fish oil, or increased fish intake, during pregnancy prevents the pregnancy-induced hypertension, prolongs gestation, increases birth weight and reduces the incidence of premature birth
– Gerrard et al, 1991, Olsen et al, 1992
Recent data support the view that the intake of DHA during pregnancy should be in the amount of at least 0.1-0.4 g/day
– Crawford, 1995
Fetal stage DHA is important for optimal nervous system development. During the last trimester of pregnancy, when the fetal demand for neural and vascular growth are greatest, there is an elevated accretion of DHA in the liver and brain of the fetus. A maternal diet high in DHA will greatly enrich the DHA concentration in the blood of the newborn infant. Even levels as low as 0.7g EPA+DHA/day during the period from 25th to 35th week of pregnancy seem to be beneficial
– Connor et al, 1995
DHA levels in maternal plasma are lower in multi-gravidae compared to primigravidae and the smaller the baby, the lower DHA-level
– Al et al, 1995
Consequently, it is therefore especially important for multi-gravidae to increase the intake of DHA.
Pre-eclampsia During pregnancy, blood lipids, triglycerides and cholesterol may rise several folds. There may also be an increase in blood pressure. The risk of developing pre-eclampsia and subsequent premature birth is increased if these, otherwise normal changes are increased above certain levels. Severe forms of pregnancy-induced hypertension have been reported to be beneficially modulated by omega-3 fatty acids
– Secher et al, 1991
 In light of their very strong hypotriglyceridemic and hypotensive effects, omega-3 fatty acids along with other nutritional factors may be significant for the prevention of pre-eclampsia. The maternal blood pressure responses depend on the ARA/EPA ratio in the vessel wall. Multi-center studies are currently in progress and the first results are expected to be available before 1997. In the meantime, it would generally seem prudent to recommend an increased intake of omega-3 fatty acids during pregnancy. EPA will benefit the mother’s heart and circulation, and DHA will definitely be good for the development of fetal brain and nervous system.
In light of their very strong hypotriglyceridemic and hypotensive effects, omega-3 fatty acids along with other nutritional factors may be significant for the prevention of pre-eclampsia. The maternal blood pressure responses depend on the ARA/EPA ratio in the vessel wall. Multi-center studies are currently in progress and the first results are expected to be available before 1997. In the meantime, it would generally seem prudent to recommend an increased intake of omega-3 fatty acids during pregnancy. EPA will benefit the mother’s heart and circulation, and DHA will definitely be good for the development of fetal brain and nervous system.
Recent studies have demonstrated that DHA supplementation during pregnancy and lactation is necessary, to prevent deficiency of the mother’s DHA status during these periods, to meet the high fetal requirement for DHA. It has been shown that premature babies have lower levels of DHA in their tissues as compared to full-term babies. Thus, supplementation of infant formula with DHA/marine oils may be necessary in order to provide them with as much DHA as that available to their breast-fed counterparts.
Feeding of infants with formula devoid of omega-3 fatty acids resulted in lack of deposition of DHA in their visual and neural tissues with adverse effects on vision and nervous systems.
According to Dr. Connor, “The signs of omega-3 deficiency in infancy are subtle, for example, omega-3 fatty acid deficiency in infants can translate into:
– impaired vision
– abnormalities on the electroretinogram (measures retinal nerve function)
– behavioural changes, such as polydypsia (excessive thirst), hyperactivity and perhaps less cognitive ability
Some of these changes have been described only in subhuman primates. So it’s clearly essential for pregnant and breast feeding women to ensure their dietary intake of omega-3 PUFA is adequate.”
Go to top of page.
Prostate Cancer
Several studies have shown an inverse relationship between blood levels of fish oils (eicosapentaenoic acid
The Swedish study involved 3,136 pairs of male twins born between 1886 and 1925. The participants completed food frequency questionnaires in 1961 and 1967 and were then followed up for 30 years. By December 31, 1997 the researchers had recorded 466 diagnoses of prostate cancer (340 fatal ones). The average age of diagnosis was 76.7 years. After adjusting for other known risk factors the researchers conclude that men who never eat fish have a two-to-threefold higher risk of prostate cancer than do men who eat moderate to high amounts. The researchers emphasize that only fatty fish such as salmon, herring and mackerel, which contain high amounts of omega-3 fatty acids (EPA and DHA), would be expected to be beneficial.
Go to top of page.
Psoriasis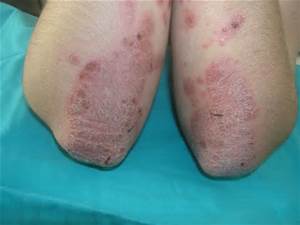
Psoriasis is a fairly common skin disease characterized by thick, silvery white scales surrounded by a red, inflamed border. Psoriasis is accompanied by high concentrations of arachidonic acid in the plaques and profound changes in the metabolism of eicosanoids leading to an increase in pro-inflammatory agents. It is known that eicosapentaenoic acid (EPA) counteracts the formation of these pro-inflammatory agents and some studies have shown that oral supplementation with fish oils benefits psoriasis patients.
A team of researchers from Austria, the Czech Republic, the Slovak Republic, Germany, and Poland now report that intravenous infusions of a fish oil emulsion is quite effective in ameliorating the symptoms of chronic plaque-type psoriasis. Their double-blind, randomized, placebo-controlled, multi-center trial involved 54 men and 29 women between the ages of 18 and 80 years who had been hospitalized with severe psoriasis. The patients were randomized into two groups. Group 1 (43 patients) received twice daily infusions of a fish oil emulsion (100 ml of a 10% emulsion infused over a period of 90 minutes) while group 2 (40 patients) received twice daily infusions of a placebo emulsion based on linoleic acid. Physicians assessed the severity of the psoriasis on days 0, 4, 7, 11 and 15 of the two-week trial.
Sixteen of the 43 patients (37%) receiving fish oil showed at least a 50% improvement in their condition at the end of the trial as compared to 9 out of 40 patients (23%) in the placebo group.
Go to top of page.
Raynaud’s Disease
Raynaud’s phenomenon is characterized by periods of disrupted blood flow in the fingers caused by exposure to cold or stress. The condition is relieved by warming the affected parts. It is estimates that about 4% of the US. Population suffers from the primary form of this phenomenon, the so-called Raynaud’s disease. Secondary Raynaud’s phenomenon occurs in association with connective tissue disease (progressive systemic sclerosis). Researcher at Albany medical college now report that supplementation with marine oils significantly reduces the symptoms of Raynaud’s disease (primary Raynaud’s Phenomenon) but has no beneficial effects in Secondary Raynaud’s Phenomenon.
Go to top of page.
Rheumatoid Arthritis
Several studies have shown that supplementation with n-3 polyunsaturated fatty acids (n-3 PUFAs) found in fish oils is beneficial for rheumatoid arthritis (RA) patients. Spanish medical researchers now report that RA patients tend to have decreased levels of n-3 PUFAs in their blood and synovial (joint) fluid. Their study involved 24 female and 15 male RA patients (median age of 64 years). Blood and joint fluid samples were collected from the patients and from a control group consisting of 28 healthy volunteers (17 male and 11 female with a median age of 61 years). All samples were analyzed to determine their fatty acid profile.
RA patients were found to have significantly lower levels of eicosapentaenoic acid (the main component of fish tissue oil) in both their blood plasma and synovial fluid. The level of alpha-linolenic acid was lower in the synovial fluid of RA patients, but not in their blood plasma. The level of docosahexaenoic acid (a major component of fish tissue oil) also tended to be lower in synovial fluids of RA patients, but not in their blood plasma.
The researchers conclude that RA patients have an abnormal fatty acid profile and a significant deficiency in certain essential fatty acids. They believe this finding may explain why supplements such as fish oils and gamma-linolenic acid (from evening primrose and borage) have been found to be beneficial in the treatment of rheumatoid arthritis.
Go to top of page.
Schizophrenia
There is evidence that schizophrenia is associated with an abnormal metabolism of unsaturated fatty acids in both blood plasma and red blood cells. This abnormality, in turn, is associated with extraordinary low levels of long-chain unsaturated fatty acids such as EPA (eicosapentaenoic acid), DHA (docosahexaenoic acid), and AA (arachidonic acid) in cell membranes.
Researchers at the Imperial College School of Medicine now report that fatty acid levels can be restored to normal and schizophrenia symptoms eliminated or at least vastly diminished by oral supplementation with EPA, the major component of fish oils. Their experiment involved a 30-year-old man who had suffered from schizophrenia for over 10 years. He had frequent (at least daily) hallucinations and also suffered from persecutory delusions and thought disorder. The patient was put on 2 grams/day of EPA and was evaluated for schizophrenia symptoms and blood plasma and red blood cell membrane levels of fatty acids at monthly intervals for 6 months. The results were spectacular. After 6 months the overall score for schizophrenia symptoms had dropped by a factor of 6 (an 85% reduction in severity). Episodes of delusions were completely eliminated and there was an 88% reduction in the number of hallucinatory episodes.
The remarkable clinical improvement in symptoms was associated with substantial increases in the levels of EPA, DHA and AA in red blood cell membranes and with significant increases in EPA and DHA levels in blood plasma. The researchers conclude that EPA supplementation is able to reverse the abnormal fatty acid profiles found in schizophrenics and that this reversal is associated with, and is likely to be the cause of, the clinical improvement.
Go to top of page.
Stroke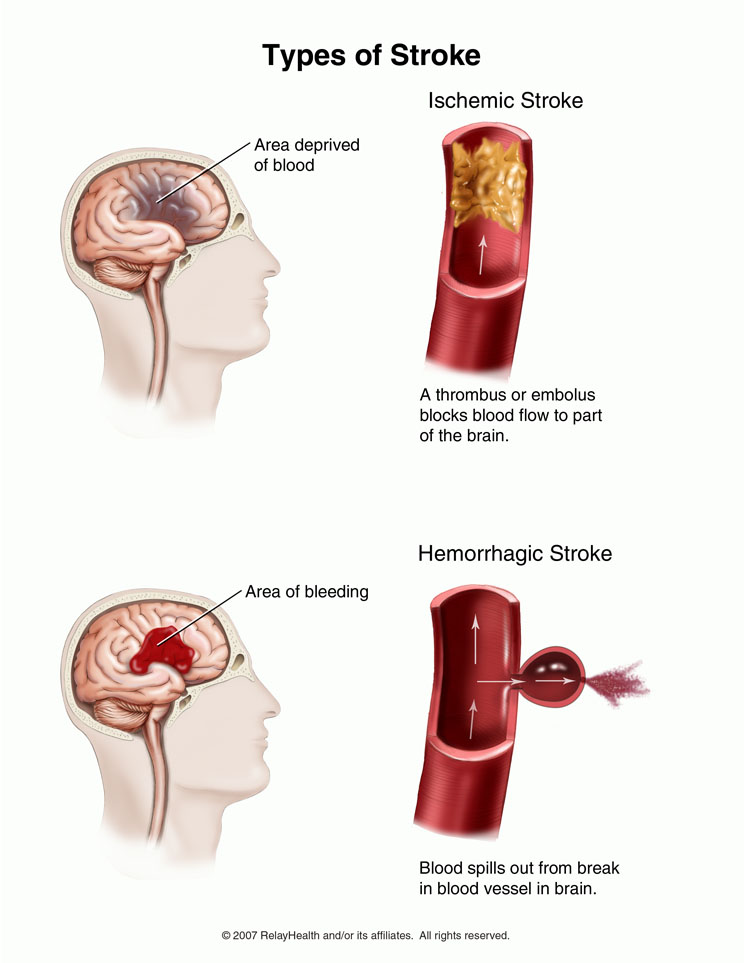
A stroke has become known as a brain attack and is the third leading cause of death in this country. A stroke cuts off oxygen to the brain causing the death of vital nerve cells. There are two types of strokes. One is called an ischemic stroke where blood flow is blocked and not enough oxygen is getting to the brain. The events leading up to this type of stroke is similar to those in heart attacks. This type accounts for two thirds of all strokes. The second type of stroke is a Hemorrhaged stroke where the artery supplying blood and oxygen to the brain bursts because of weakness in the vessel wall, usually caused by high blood pressure. The nerve cells that are normally supplied by the burst artery are deprived of oxygen and begin to die. Hence reducing elevated blood pressure has become the first line of defense to avoid a hemorrhaged stroke. Large doses of marine oil (Omega 3 Fatty Acids) have been shown to reduce blood pressure and also reduce blood clot formation. Dutch researchers have confirmed a line between fish consumption (as little as one 3 ounce serving per week), and a reduced risk of stroke, Nothing marine oils ability to retard coagulation, a thickening of the blood that can lead to stroke inducing clots.
Go to top of page.
Ulcerative Colitis
Ulcerative colitis, a common form of inflammatory bowel disease, is accompanied by an increased level of leukotriene B4 in the lining of the colon. Fish oils are known to inhibit the synthesis of leukotrienes and it has therefore been postulated that they might be beneficial in the treatment of ulcerative colitis. Researchers at the Veterans Affairs Medical Center have just released the results of a study aimed at testing this hypothesis.
The study involved 11 male patients aged 31 to 74 years old who had been diagnosed with ulcerative colitis. The patients were randomized into two groups with one group receiving 15 fish oil capsules (providing 2.7 grams of eicosapentaenoic acid (EPA) and 1.8 grams of docosahexaenoic acid (DHA) daily); the other group received placebo capsules (olive oil). After 3 months on the supplements all participants underwent a 2-month wash-out period and were then assigned to the opposite treatment to what they had received during the first stage for another 3 months. Clinical evaluations of all patients were performed at the start of the study and every month thereafter.
 Evaluation of the patients’ clinical data at the end of the treatment periods showed a significant beneficial effect of fish oil supplementation. The mean disease severity scores for the patients on fish oil declined by 56% as compared to 4% for the placebo group. Eight of the 11 patients (72%) were able to markedly reduce or totally eliminate their use of anti-inflammatory medication and steroids while taking the fish oils.
Evaluation of the patients’ clinical data at the end of the treatment periods showed a significant beneficial effect of fish oil supplementation. The mean disease severity scores for the patients on fish oil declined by 56% as compared to 4% for the placebo group. Eight of the 11 patients (72%) were able to markedly reduce or totally eliminate their use of anti-inflammatory medication and steroids while taking the fish oils.
The researchers conclude that fish oil supplementation results in a marked clinical improvement of active mild to moderate ulcerative colitis.
Go to top of page.
Vision Disorder
Dr. Barbara Levine, Professor of Nutrition in Medicine at Cornell University, sounds the alarm concerning a totally inadequate intake of DHA (docosahexaenoic acid) by most Americans. DHA is the building block of human brain tissue and is particularly abundant in the grey matter of the brain and the retina. Low levels of DHA have recently been associated with depression, memory loss, dementia, and visual problems.
DHA is particularly important for fetuses and infants; the DHA content of the infant’s brain triples during the first three months of life. Optimal levels of DHA are therefore crucial for pregnant and lactating mothers. Unfortunately, the average DHA content of breast milk in the United States is the lowest in the world, most likely because Americans eat comparatively little fish. Making matters worse is the fact that the United States is the only country in the world where infant formulas are not fortified with DHA. This despite a 1995 recommendation by the World Health Organization that all baby formulas should provide 40 mg of DHA per kilogram of infant body weight. Dr. Levine believes that postpartum depression, attention deficit hyperactivity disorder (ADHD), and low IQs are all linked to the dismally low DHA intake common in the United States.
Dr. Levine also points out that low DHA levels have been linked to low brain serotonin levels which again are connected to an increased tendency to depression, suicide, and violence.
DHA is abundant in marine phytoplankton and cold-water fish and nutritionists now recommend that people consume two to three servings of fish every week to maintain DHA levels. If this is not possible, Dr. Levine suggests supplementing with 100 mg/day of DHA. Source: Cornell University
Go to top of page.
Disclaimer Statement


